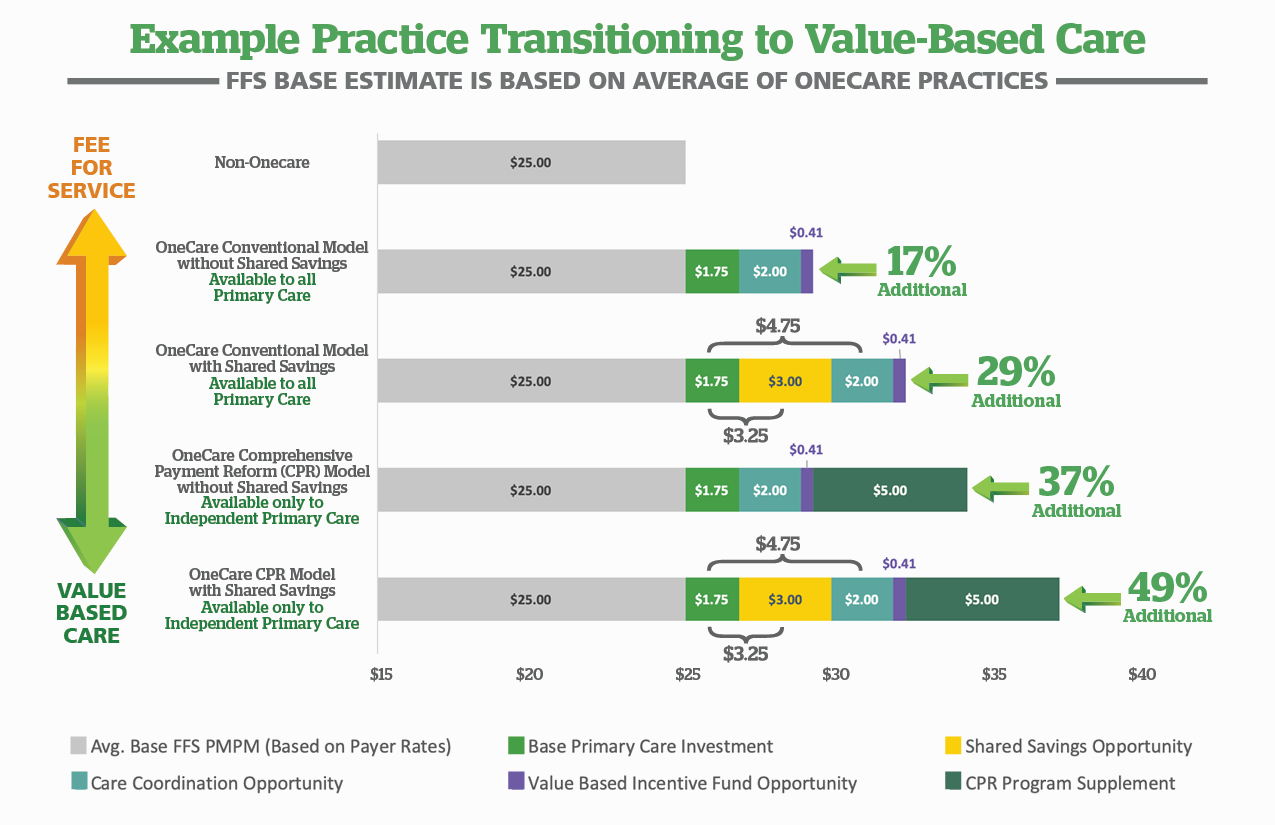
Payment Reform
OneCare Vermont’s payment reform core capability is carefully designed to improve the quality of care by changing the way we pay for care.
OneCare pays fixed monthly amounts to providers to care for their patients—helping shift away from the fee-for service model that rewards for more care, to focusing on delivering the best care through a value-based model. The vision for value-based care is better health outcomes and a flattened cost curve for health care spending. When providers are reimbursed for value instead of volume, over time, they can change the way they deliver health care and invest in activities that are designed to lead to better health outcomes—primary care, health prevention, early identification of disease, and the right treatment at the right time. Savings earned by providers in the network can be re-invested into practices, such as in primary prevention efforts or additional care coordination services to support people with chronic illness.
The idea of a fixed payment for a population of patients can make some wonder if providers will avoid providing necessary care as a means to stay within their fixed budget. In fact, the opposite is true. Providers under fixed payment programs are incentivized to make sure they are ordering the right tests, services, procedures—and also exploring social determinants of health that may need to be addressed like food access, housing, and social connection—as a means to prevent more significant health issues later on.
How Payment Reform Works
The fixed amounts participating providers receive through OneCare’s payment reform model are based on historical fee-for-service spending to smooth the transition to value-based payments. OneCare offers payment reform for hospitals and independent primary care.
Hospitals
Hospital payment reform is important because hospital care is often the most expensive care. OneCare works with Vermont hospitals to provide predictable, fixed monthly payments for the patients they serve. The monthly payment model aims to stabilize hospital revenue and incentivize investment in preventive care and care coordination for people with chronic illnesses. If this transition is successful, it will result in a healthier population and fewer costly hospital stays.
Independent Primary Care
OneCare works with independent primary care providers to support the transition to value-based care. Independent primary care practices receive financial resources that aim to shift focus to the care that’s right for their patients rather than billable services. OneCare offers a fixed payment to independent primary care practices, much like the hospital fixed payments, that are not part of a hospital or health system through its Comprehensive Payment Reform (CPR) program.
OneCare Vermont’s own “Comprehensive Payment Reform” pilot project—aptly abbreviated “CPR”—changes the payment method from fee-for-service to a fixed monthly payment with which we can focus on taking the best care of the patients in our practices.
This is the first real investment our independent primary care practices have seen. It has allowed us to provide better team-based care within our offices. We now have dedicated care coordinators who can help patients navigate complicated health and social situations. We have implemented more mental health and social services in our offices where patients can access them on site. We fully expect that this more integrated approach will have a positive effect on the health of our patients and communities
Payment Reform Link to Two Other Core Capabilities

Core Capability #1:
Network Performance Management
This core capability includes the contracts OneCare puts in place between payers and providers, shifting to paying for value instead of volume.
Once contracts are put in place, this core capability also works to support providers to succeed in their contracts through care coordination and quality improvement.

Core Capability #2:
Data and Analytics
OneCare Vermont makes use of data and analytics by measuring health care cost, quality, and utilization across an entire population of patients to help providers identify which Vermonters need outreach and which areas of care delivery to improve.
OneCare data and analytics help providers prioritize their efforts on quality improvement that will have the biggest impact Vermonters’ health and on the cost of care.